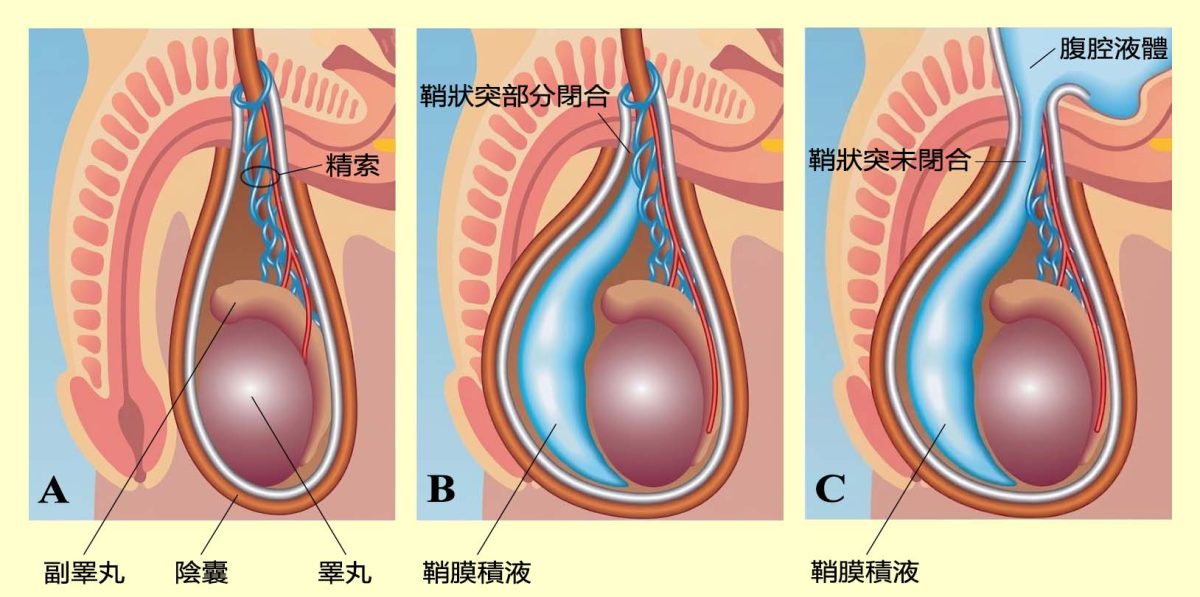
The processus vaginalis is a pouch-like outgrowth of the peritoneum that extends through the inguinal canal into the scrotum during embryonic development. Its physiological role is to guide the descent of the testis, and it normally closes spontaneously before or shortly after birth. If it closes only partially, fluid accumulates between the two layers of the tunica vaginalis in the scrotum, resulting in a non-communicating hydrocele. If it fails to close completely, peritoneal fluid can flow into the scrotum and collect between the two layers of the tunica vaginalis, forming the clinically common communicating hydrocele (Figure 1). In adults, hydroceles are usually associated with inflammation, trauma, infection, or tumors, leading to excessive secretion of fluid by the tunica vaginalis or impaired fluid reabsorption.
Clinical symptoms include painless scrotal enlargement and a sense of heaviness or dragging. If the hydrocele becomes very large, it may cause difficulty with movement. In some cases, it may be accompanied by acute complications such as epididymitis, testicular torsion, or pyocele. Long-standing fluid accumulation can exert physical pressure on the spermatic cord vessels, reducing testicular blood perfusion, altering the temperature-regulating mechanism within the scrotum, and potentially impairing spermatogenesis or causing testicular atrophy. In addition, hydrocele may stretch and thin the scrotal skin; chronic friction may lead to redness, eczema, or ulceration of the scrotal skin. If a communicating hydrocele is left untreated, the patent processus vaginalis may progress to an inguinal hernia, or even a strangulated hernia.
The widely accepted definitive treatment in modern medicine is hydrocelectomy, also known as excision of the hydrocele sac (tunica vaginalis). In cases of communicating hydrocele, high ligation is required to close the patent processus vaginalis. An alternative treatment is needle aspiration with sclerotherapy. After aspirating the fluid with a needle, a sclerosing agent is injected to cause adhesion of the tunica vaginalis layers. However, this method has a recurrence rate of over 80% and may cause pain or epididymal inflammation. Therefore, it is usually reserved for elderly patients who are not suitable candidates for surgery.
Purpose of Surgery
- During surgery, the physician can directly inspect the testis and rule out hidden testicular tumors or severe inflammation. Removal of a large amount of accumulated fluid immediately relieves pressure on the testis and spermatic cord vessels, improves local blood circulation, and protects testicular function. Simultaneous ligation of the patent processus vaginalis effectively prevents the development of an inguinal hernia. Surgery also improves discomfort and psychological stress caused by scrotal enlargement during dressing, walking, or exercise.
Type of Anesthesia
Our clinic uses dual local anesthesia, similar to the anesthesia technique used for penile-related procedures. Local anesthetic is injected only into the scrotal or inguinal surgical site. During the procedure, the patient remains awake and pain-free, and may use a mobile phone or Bluetooth earphones.
Surgical Wound
A single incision, approximately 3 cm in length, is made in the scrotum or groin.
No hospitalization is required. After surgery, there is no need for prolonged observation, and patients may walk and return home to rest freely.
Is Hospitalization Required?
No hospitalization is required. After surgery, there is no need for prolonged observation, and patients may walk and return home to rest freely.
Surgical Technique
The procedure is performed with the patient in the supine position. Precise dual local anesthesia is administered at the surgical site to prolong the effective anesthetic duration. An appropriate site on the scrotum or groin is selected, and a straight incision is made. The fascial tissue beneath the wound is carefully dissected while preserving adjacent blood vessels and normal tissues. The hydrocele fluid is drained, and the excess tunica vaginalis is either excised or everted and sutured posteriorly to remove the membrane responsible for fluid production. Finally, the wound is closed with fine sutures and covered with sterile gauze dressing.
Features of Surgery at Our Clinic
- Dual local anesthesia Single incision No hospitalization required No electrocautery for hemostasis, minimizing tissue damage. If electrocautery is used to control bleeding from blood vessels during surgery, it may injure nearby arteries or nerves, leading to abnormal sensation, numbness, or chronic pain. Arterial injury may also result in local ischemia and risk of tissue necrosis. Many medical studies have reported that electrocautery damages local tissue; the cauterized area loses blood circulation, reducing bacterial resistance and increasing the risk of wound infection and inflammation. Even in the absence of infection, it may adversely affect wound healing. Use of refined microsurgical techniques to improve surgical safety and reduce potential complications. Our clinic applies the same principles to other related procedures, including microscopic circumcision, hernia repair, varicocelectomy, penile curvature correction, modified penile venous stripping, penile prosthesis implantation, testicular prosthesis implantation, vasectomy, and dorsal penile nerve block, making these procedures relatively safe.
Prognosis
After surgery, there may be some swelling, pain, or discomfort at the wound site. These symptoms are usually well controlled with oral pain medication and gradually subside. As with any surgery, there is a risk of infection; therefore, prophylactic antibiotics are administered before and after the operation. Possible complications include:
- Scrotal hematoma (2–18%)
- Wound infection (2–5%)
- Chronic scrotal pain (2–10%)
- Recurrence of hydrocele (1–5%)
- Testicular atrophy (<1%)
- Vas deferens injury (<1%)
All surgical and medical procedures carry some degree of risk. However, with skilled and meticulous surgical technique, the incidence of complications can be reduced to a minimum.
Conclusion
A hydrocele refers to the accumulation of fluid within the tunica vaginalis cavity. In addition to causing scrotal enlargement and a sensation of heaviness, a large hydrocele may interfere with mobility and may sometimes be associated with acute complications such as epididymitis, testicular torsion, or pyocele. Long-standing untreated fluid accumulation increases physical pressure and disrupts temperature regulation, which may impair spermatogenesis and lead to testicular atrophy.
Compared with needle aspiration, which has an extremely high recurrence rate, hydrocelectomy completely eliminates the space where fluid accumulates. In pediatric patients, surgery also allows simultaneous ligation of the patent processus vaginalis, effectively preventing inguinal hernia. It offers a high cure rate and low recurrence rate. For patients with significant symptoms or progressive enlargement, timely surgery not only relieves physical compression but also helps protect male reproductive health and improve confidence in daily and social life.
References
- Hsu GL, Hsieh CH (謝政興), Chen HS, Ling PY, Wen HS, Liu LJ, Chen CW, Chua C. The advancement of pure local anesthesia for penile surgeries: can an outpatient basis be sustainable (純粹局部麻醉施行陰莖手術的新進展)? Journal of Andrology. 28(1):200-205, 2007.
- Hsu GL, Zaid UX, Hsieh CH (謝政興), Huang SJ. Acupuncture assisted local anesthesia for penile surgeries (針灸輔助局部麻醉下施行陰莖手術). Translational Andrology and Urology. 2(4):291-300, 2013.
- Hsu GL, Hsieh CH (謝政興), Wen HS, Hsu WL, Chen YC, Chen RM, Chen SC, Hsieh JT. The effect of electrocoagulation on the sinusoids in the human penis (電燒止血對於人類陰莖海綿體的影響). Journal of Andrology. 25(6):954-959, 2004.
- Partin, A. W., Peters, C. A., Kavoussi, L. R., Dmochowski, R. R., & Wein, A. J. (Eds.). (2020). Campbell-Walsh-Wein urology (12th ed.). Elsevier.
- European Association of Urology. (2026). EAU guidelines on paediatric urology. EAU Guidelines Office. https://uroweb.org/guidelines/paediatric-urology
- American Urological Association. (2021). Diagnosis and management of inguinal hernias and hydroceles. American Urological Association Education and Research, Inc.
- Özkan, B. A., Öztürkkan, S., & Gözüküçük, R. (2024). Long-term outcomes and quality of life after hydrocelectomy: A comparative study of Jaboulay vs. Lord’s technique. Journal of Urology, 211(5), 842–850.
